Direct, image-based targeting under general anesthesia without the use of microelectrode recording (MER) or intraoperative test stimulation, also known as asleep DBS surgery, is becoming more popular as a result of advances in neuroimaging.
Retrospective comparisons comparing awake surgery and sleep surgery with MER have demonstrated similar short-term efficacy with the potential for fewer problems in sleeping cohorts, in place of randomized control trials. Although patient-specific factors may also be used to guide the decision regarding which technique may be most appropriate and tolerable to the patient, awake DBS using MER must demonstrate more durable outcomes with less stimulation-induced side effects and lead revisions in order for its users to remain justifiable in the absence of long-term outcome data.
Surgery for deep brain stimulation (DBS) is a viable Parkinson’s disease treatment (PD). Up until now, intraoperative test simulations have been used to do awake surgery most frequently. The position of the electrode tip has recently been confirmed during awake surgery under general anesthesia (GA) using intraoperative magnetic resonance imaging (iMRI) or computed tomography (iCT).
What Happens In Awake Surgery Brain And Sleep Surgery?
Mapping the borders of deep brain nuclei that were difficult or impossible to see on traditional imaging sequences was the goal of awake surgery using MER. By identifying target boundaries in regard to important white matter tracts, diffusion tensor imaging (DTI) may be useful in sleeping DBS, as shown by the agreement between electrophysiological tissue activation and the separation between visible corticospinal tract fibers. Therefore, any deep brain structure that can be seen radiographically is a candidate for asleep deep brain stimulation. Depending on the center, asleep DBS surgery has often been carried out using either intraoperative MRI guidance (iMRI) or intraoperative CT (iCT) confirmation. These two strategies vary not just in the imaging modality they employ but also in how the imaging is put to use. Typically, an iCT is performed after the DBS lead has been positioned at the intended stereotactic target as a confirming procedure. The preoperative MRI and iCT images are then combined, and the stereotactic position of the lead is established using the results of the CT-MRI fusion.
Targeting Accuracy
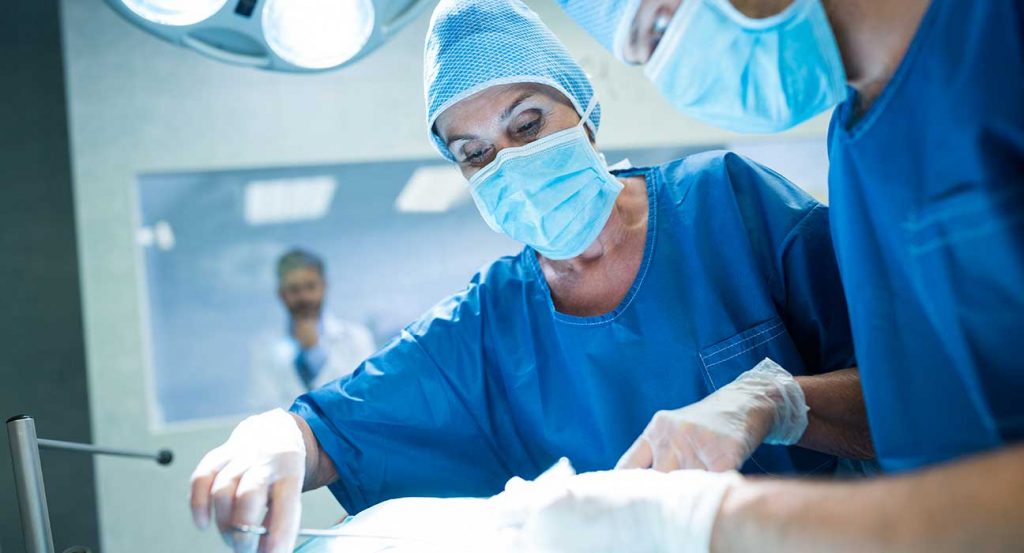
Theoretically, awake DBS surgery employing MER yields better results than asleep DBS surgery when stereotactic precision in reference to the designated target is used. Therefore, the lead’s stereotactic precision in regard to the intended target is essential. The anatomic target is further optimized by electrophysiological mapping during awake DBS surgery. There is a dearth of published evidence on whether MER target refinement causes a large deviation of DBS lead placement, where the divergence is, on average, bigger than the intrinsic targeting error associated with DBS lead placement itself.
Conclusion
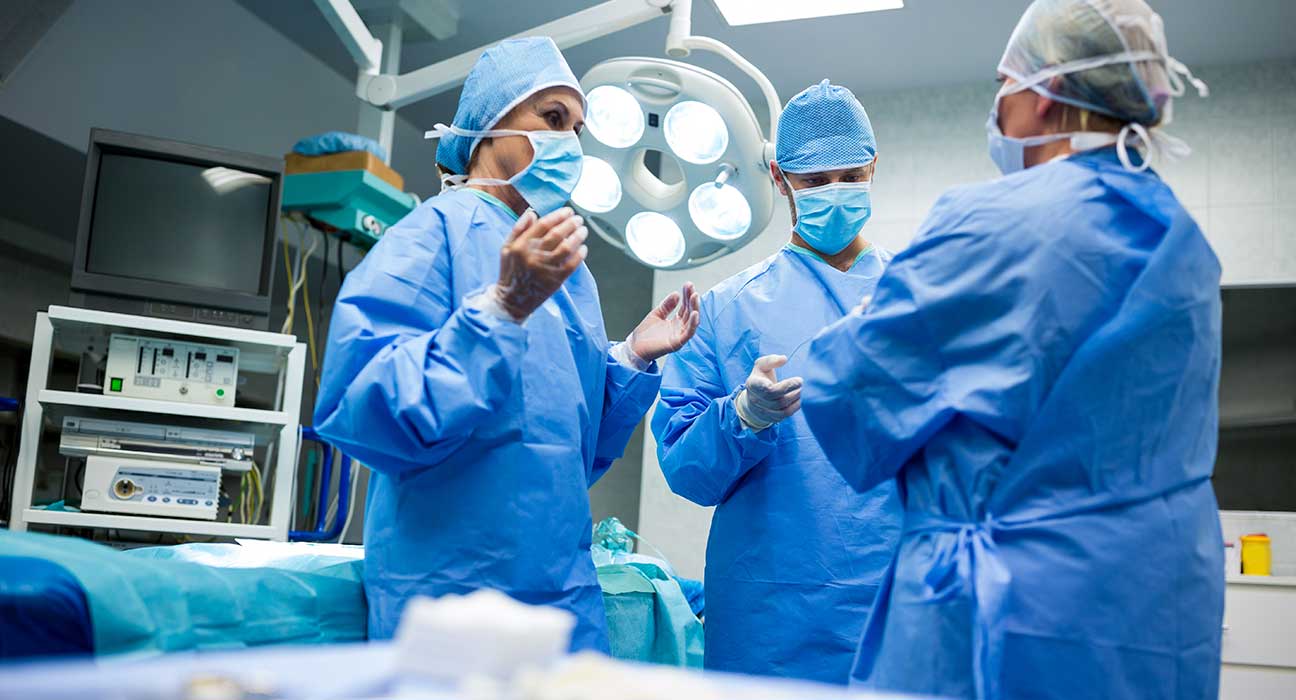
While awake DBS may result in fewer treatment-related adverse effects, DBS under general anesthesia may result in lower overall complication rates. However, there were no appreciable variations in clinical motor outcomes between the two approaches. Because of this, patients who are not candidates for typical awake DBS or who prefer the sleeping alternative can be considered for DBS under general anesthesia at centers with experience.

Leave feedback about this